 However, his primary dentist could not connect the existing bruxism to the patient’s complaints about teeth 36 and 46. For a brief period (1.5 years after the first onslaught of pain and 2 weeks before endodontic treatment), he wore a bite splint. When explicitly asked by the attending dentist of the university hospital, the patient confirmed having had a lot of stress during the phase of the pain development due to the completion of his studies, as well as having pressed a lot at night (Fig. At that time, the teeth already appeared avital. 3) was made by the primary dentist, a diagnosis of apical periodontitis on teeth 36 and 46 was finally established, and endodontic treatment was initiated. Remission of pain followed, but 2.5 months later the pain started again. 1) and gave antibiotics (Clindasaar, 600 mg, 1–1-1), but did not start any treatment, being unable to establish a diagnosis. An emergency service dentist took 2 x-rays (Fig. A short period of percussion pain (2 days) occurred and, once again, disappeared. About 1.5 months later, the same pain started again on both teeth (36 and 46). Referral to an otolaryngologist prescribing an antibiotic (Amoxicillin 1000 mg, 3 times a day for 7 days) without diagnosis followed, resulting in complete remission of the pain. The primary dentist was unable to identify an odontogenic cause for the complaints. The patient did not have any pain on release of pressure. The percussion test done by the primary dentist was negative and the sensibility test reduced. The patient described a short period (2 days) of percussion pain, which then disappeared. Simultaneous earache and temporomandibular joint pain occurred. The pain was pulling, diffuse, radiating, difficult to localise and, before going to sleep, pulsating. 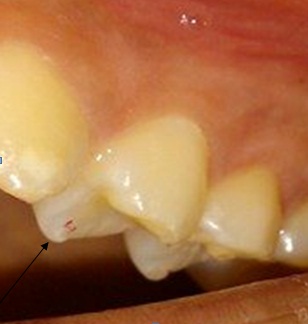
During anamnesis, the patient reported that complaints first appeared 1.5 years ago on the right side (tooth 46). No external resorption, root canal or pulp chamber perforation was apparent. Clinically and radiologically no anomalies, pulp calcifications, or formation defects of the hard tooth tissue could be detected. Furthermore, a slight bulging elastic swelling could be observed in the vestibulum. Teeth 36 and 46 each showed a 10 mm pocket, with bleeding on probing the vestibular-central. The periodontal screening index was unremarkable, with no signs of periodontal disease. Clinical examination of both teeth revealed an increased tooth mobility and bifurcation at a probing depth of 4 mm. The teeth had no fillings or caries, no trauma or accident had occurred, the patient did not have any periodontal problems, and also had no pain. The cause of apical periodontitis could not be determined by the primary dentist. 
Within the last six months, several changes of medication had taken place. Endodontic treatment had already been initiated, but apical osteolysis was increasing on both teeth. Ī 28-year-old healthy male patient was referred by his primary dentist to the Clinic of Operative Dentistry, Periodontology and Preventive Dentistry, Saarland University in Homburg, Germany with apical periodontitis on teeth 36 and 46. 
Experimental consequences of occlusal trauma to the pulp have already been described. As far as the authors know, this is the first described clinical case of apical periodontitis caused purely by bruxism. Typical dental problems caused by bruxism are abrasion, chipping of teeth and/or prosthetic restorations, orofacial pain, teeth sensitivity, pulpal pathology, fractures of teeth and restorations, and damage of implants. Stress, personality characteristics, smoking, disease, trauma, genetics, alcohol, caffeine consumption, illicit drugs and medications may be involved in its aetiology. describe a 6–20% prevalence of bruxism in the population in all age groups. In their bibliographic review Demjaha et al. Considering neuromuscular activity, a toned, periodic and combined type of bruxism can be classified. A multifactorial etiopathogenesis is discussed and a mild, moderate and severe bruxism distinguished. īruxism is described as a nightly orofacial motor function leading to an occlusal trauma, fractures of teeth, headache, muscle pain and periodontal problems. The main objective of endodontic treatment is to preserve the tooth in the oral cavity in healthy conditions. Recovery, repair, or necrosis may follow. Trauma can injure a dental pulp by damaging apical blood vessels (from luxation, avulsion injuries, or rupture of intra-pulpal blood vessels), leading to an intra-pulpal haemorrhage. 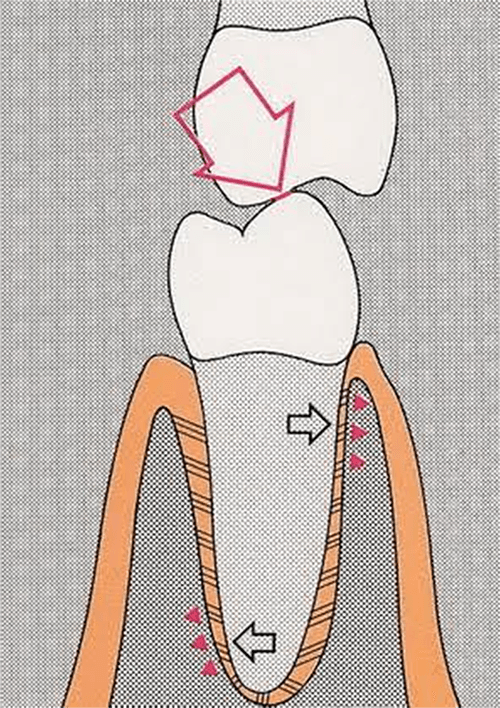
A variety of important factors can account for this, including short and long-term irritations (initiated during treatment) or trauma. The prevalence of apical periodontitis is as high as 34–61%, it increases with age and is often associated with pulp diseases. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
